Technical terms
Antiarrhythmic drugs
A group of medicines used to regulate and control the heart’s rhythm. They may be of use in specific situations in people with LQTS (e.g. mexiletine) although they are not of proven benefit in preventing sudden death. Ajmaline and flecainide are used in tests used to diagnose Brugada Syndrome.
Aorta
The major blood vessel that leaves the left side of the heart. It supplies blood to the body.
Aortic valve
The valve through which blood passes from the heart into the aorta. A bicuspid valve (a valve that has only two cusps or ‘flaps’) fails to open properly due to the absence of the third cusp and can narrow up due to repetitive damage.
Arrhythmia
A disturbance of the heart’s rhythm. A ‘ventricular’ arrhythmia can be lifethreatening.
Asystole
When the heart’s rhythm stops completely because there is no electrical activity.
Atrium
One of the two top chambers of the heart. (The plural of ‘atrium’ is ‘atria’.)
Autopsy
A post-mortem examination of a dead body.
AV block
See ‘heart block’.
AV node
Atrioventricular node. The part of the heart that lies between the top chambers (‘atria’) and bottom chambers (‘ventricles’). It regulates the transmission of electrical impulses from the natural pacemaker in theatrium to the ventricle. It helps to prevent the heart from pumping too fast if the impulses from the atrium become too rapid.
Bradycardia
Slowing of the heart rate.
Cardiac
‘Of the heart’ or ‘belonging to the heart’.
Cardiac arrest
The state of the heart when it is pumping so erratically or ineffectively that there is no significant blood pressure to supply the heart and brain. If the problem is not resolved within two minutes there will be permanent brain damage, and if left untreated the person will quickly die. This is the mechanism by which the channelopathies can cause sudden death.
Cardiologist
A doctor who specialises in the heart.
Cardiomyopathy
Disease of the heart muscle, which is usually inheritable.
Cardiopulmonary exercise test
An exercise test that monitors the consumption of oxygen, using a set of breathing tubes.
Cervical sympathectomy
A form of surgery that is useful for some people with LQTS. It reduces the amount of adrenaline and its by-products produced and delivered to the heart by certain nerves (the left cervical ganglia). It involves operating on the left neck and removing or blocking these nerves, which are not essential to normal function. The procedure can be relatively short but it does need a general anaesthetic.
Congenital heart disease
Disease of the heart, present from birth.
Coronary artery disease
Narrowings and blockages of the arteries supplying the heart muscle, due to ‘furring of the arteries’. Also known as ‘arteriosclerosis’.
Coroner
The government-appointed legal person responsible for ensuring that no foul play has occurred when an unexpected death happens.
Defibrillator
A device used if a person has a cardiac arrest. It may be able to return the heart to a normal rhythm by delivering an electrical ‘shock’ through the chest wall.
Delta wave
The ECG feature characteristic of Wolff-Parkinson-White (WPW) Syndrome.
DNA
The genetic code from which proteins – ‘the building blocks of life’ – are made. We all receive a copy of half of each of our parents’ DNA when the egg and sperm meet to conceive a new human being.
Ectopic beat
An ‘extra’ beat which occurs when the heart activates prematurely, disrupting its normal rhythm. The heart’s natural pacemaker resumes its normal control after a brief pause. Most of the time the person does not notice these extra beats but, if they do become aware of them, the sensation depends on how close the ectopic beat occurs to the preceding normal beat. If it is close, only the pause might be noticed. If it occurs further away, it might be felt as an extra beat from the heart, making the rhythm feel irregular or erratic.
ERSCD
Exercise-related sudden cardiac death. See ‘SCD’ below.
Gene
The segment of DNA responsible for the production of a specific substance such as a protein that in turn forms the basis for the body to exist and function.
Heart attack
When the heart muscle is damaged by an artery becoming blocked and depriving part of the heart of oxygen. This is caused mainly by coronary artery disease. (A heart attack is also called a ‘myocardial infarct’.)
Heart block
A failure of the heart’s electrical impulses to conduct properly from the top chambers (atria) to the bottom chambers (ventricles) via the atrioventricular (AV) node. The severity of the condition and its associated risk can vary.
Figure 9: ICD (implantable cardioverter defibrillator).
An ICD is similar to a pacemaker but the lead to the ventricle is larger, to allow it to deliver a larger shock to the heart when necessary.
Implantable cardioverter defibrillator (ICD)
A metal electronic device similar to a pacemaker (see below). It can regulate the rhythm of the heartbeat, like a pacemaker does. If a dangerous arrhythmia occurs, the ICD can deliver a shock to the heart. Some people have described the shock as feeling like having a ‘kick in the chest’. An ICD is larger than a pacemaker and may have to be positioned under the chest wall muscle at the left shoulder. The procedure usually takes 1½ to 2 hours and may require a general anaesthetic. The ICD clinic checks are needed once every 3 to 6 months. The battery lasts up to 5 years. When a new battery is needed, the box containing it can be replaced easily.
Ion
A chemical substance (such as sodium or potassium) that carries an electrical charge and forms the basis of the movement of electricity through the heart muscle.
Ion channel
The route that ions take in and out of the heart muscle cells to allow movement of electricity.
Mitral valve
The valve on the left side of the heart, between the atrium and ventricle. Mitral valve prolapse (MVP) When the heart is seen on an echocardiogram, the mitral valve can appear ‘floppy’. This is very common, and affects around 1 or 2 in every 20 people. It can become more severe and the valve can become thickened and leaky. Only in rare cases it can be inherited in a family and may be associated with arrhythmias and sudden death.
Murmur
The sound of the turbulent flow of blood in the heart, sometimes due to leakage through or narrowing of valves. It can be heard through a stethoscope.
Mutation
An abnormality or ‘mis-spelling’ of the DNA code that causes its eventual product (usually a protein) to function abnormally, which in turn is responsible for a disease. A ‘sporadic’ mutation is not inherited from a parent’s DNA but occurs due to damage to the DNA after the egg or sperm that forms a human embryo is made.
Figure 10:Pacemaker.
The leads are connected both to the top chamber (atrium) and the bottom (ventricle) chamber.
Pacemaker
A small metal electronic device with internal batteries. It sits under the skin at the left shoulder. It is attached to the top and bottom chambers of the heart by two electrical leads that are inserted via the large veins near the shoulder. These leads both monitor the heart rhythm and allow treatment to be delivered to the heart. Sometimes only one chamber (the ventricle) is connected. A pacemaker can be inserted under local anaesthetic through a small 2-inch cut in the skin. The procedure takes between 45 minutes and 1 hour.
The device is programmed to pre-vent the heart from slowing down too much by giving tiny imperceptible shocks that activate the heart, independently from the heart’s natural pacemaker. The pacemaker’s battery, the leads and the programming are monitored once every 6 to 12 months in a Pacing clinic, using a special magnet and computer software. The battery lasts 5-10 years. When a new battery is needed, the metal box is replaced – a simple procedure that can be performed through the old scar.
Pathologist
A doctor trained to examine the body after death, and samples of its organs, in order to diagnose any abnormalities.
Post-mortem
The examination of a dead body by a pathologist.
Prognosis
A patient’s outlook. In this context it means the likelihood of any lifethreatening events.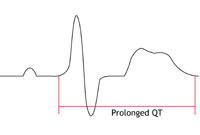
Prolonged repolarisation
When repolarisation is slower than normal, the time taken for it to occur is described as prolonged. This can be represented on the ECG by abnormalities of T waves and an increase in the QT interval (picture – right).
Pulmonary embolus (PE)
In certain circumstances a large clot can form in the deep veins of the legs – for example after long periods of immobility. The clot can dislodge and travel though the veins to the heart where it can block the arteries supplying the lungs and stop the flow of blood to the body. This can cause a sudden collapse and a rapid death. (Also called ‘thromboembolism’.)
QT interval
An ECG measure of repolarisation from the beginning of the QRS to the end of the T wave.
Repolarisation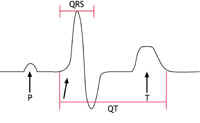
The electrical resetting of the heart muscle ready for its next activation. The time taken is measured by the QT interval (picture – right).
RF ablation
The use of high frequency radio waves to ‘burn’ away small areas of heart tissue such as the extra or ‘accessory’ pathways seen in Wolff-Parkinson-White Syndrome.
SCD Sudden cardiac death.
A death is described as sudden when it occurs unexpectedly, spontaneously and/or even dramatically. If the death is due to heart disease it is called Sudden Cardiac Death (SCD). Some will be unwitnessed or occur during sleep, while others occur during or immediately after exercise (exercise-related sudden cardiac death or ERSCD).
Stethoscope
A piece of equipment which a doctor uses to listen to the heart and chest.
Syndrome
A collection of medical features of an illness that make it a distinctive condition.
Tachycardia
A rapid heart rate.
Thromboembolism
See ‘pulmonary embolus’ above.
Toxicology
The scientific study of the effects of substances (drugs and chemicals) on the body and mind.
Vasovagal Syndrome
A disorder of the nerves supplying the blood vessels and heart that can result in dizzy episodes or blackouts. This is due to sudden drops in blood pressure because of rapid opening up (‘dilatation’) of the arteries with or without sudden slowing of the heart rate. It is usually harmless although blackouts may place the person in dangerous situations. Treatment can involve tablets and/or a pacemaker.
Ventricles
The two bottom chambers of the heart.
Ventricular
From, or belonging to, the ventricle.
Wolff-Parkinson-White Syndrome (WPW)
In this condition there is an abnormal pathway electrically connecting the top (atrium) and bottom (ventricle) chambers of the heart that can be extremely difficult to detect at an autopsy. It can, however, be diagnosed on the ECG as a ‘delta wave’ although it may not always be present and may require an ‘adenosine test’ (see cardiac tests) and/or an ‘electrophysiological study’ (see cardiac tests) to confirm its presence. It can by-pass the usual electrical regulation of the AV node and cause an abnormally rapid conduction of electrical impulses from the atria to the ventricles. In a small proportion of cases this can be severe enough that it leads to a cardiac arrest. It is rare that this condition is inherited but if so it is usually accompanied by other conditions such as unusual forms of hypertrophic cardiomyopathy.



